Responsum for CKD
{{user.displayName ? user.displayName : user.userName}}
{{ user.userType }}

If you’ve recently been diagnosed with chronic kidney disease, here’s a breakdown of essential disease information to help you make health and lifestyle decisions.
Living with, or being at risk for, chronic kidney disease (CKD) can feel overwhelming at first. There are new terms, tests, and lifestyle changes to understand. But here’s the good news: once you understand what CKD is and how it affects your body, you’re in a much better position to take control of your health.
This article is based on guidance from trusted organizations like the National Kidney Foundation and is designed to help you understand CKD in a clear and practical way.
Your kidneys are small, but they do a lot of heavy lifting.
Every day, they filter your blood to remove waste and extra fluid, which leaves your body as urine. But that’s just part of the job. Your kidneys also:
When you have chronic kidney disease (CKD), your kidneys become damaged over time (for at least 3 months) and can’t do these jobs as well as they should.
CKD usually develops slowly, and often silently. Many people don’t notice symptoms until the disease is more advanced. That’s why understanding your risk and getting tested early matters so much.
In the early stages, CKD may not cause any noticeable symptoms. As it progresses, you might start to notice changes like:
In more advanced stages, symptoms can become more serious, including:
The tricky part? These symptoms can be subtle—or mistaken for other conditions.
CKD can affect anyone, but some people are at higher risk. The most common risk factors include:
CKD can also be caused by other conditions, such as:
Here’s a stat that usually gets people’s attention: about 37 million adults in the U.S. have CKD—and most don’t know it.
The good news? Detecting CKD is actually pretty simple.
To check your kidney health, your doctor typically uses:
👉 In general:
And importantly, these results need to be present for at least 3 months to confirm CKD.
CKD is divided into 5 stages based on your eGFR:
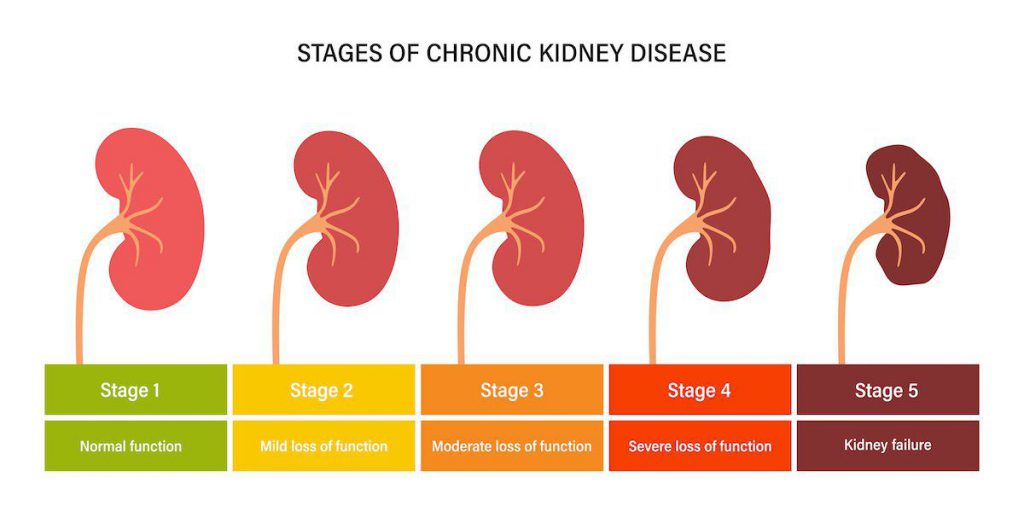
Your stage helps guide your treatment plan—but it’s not the whole story. Your symptoms, overall health, and other conditions matter just as much.
Learn more about your stages here:
Understanding How Your CKD Progression is Measured.
As CKD progresses, it can affect many parts of your body. Some common complications include:
This is why CKD management isn’t just about your kidneys—it’s about your whole-body health.
There’s no one-size-fits-all approach to CKD, but treatment usually focuses on four key goals:
Managing conditions like diabetes or high blood pressure is critical.
Medications like ACE inhibitors, ARBs, SGLT2 inhibitors, or nsMRAs may help protect kidney function.
CKD increases your risk of heart disease, so managing cholesterol and blood pressure is essential.
This may include treating anemia, balancing minerals, or addressing acid levels in your blood.
Small changes can go a long way:
👉 Avoid certain pain medications (NSAIDs like ibuprofen), unless your doctor says otherwise—they can harm your kidneys.
CKD can feel complex—but it doesn’t have to stay that way.
Once you understand what’s happening in your body, the tests your doctor orders, and the steps you can take, things start to feel a lot more manageable. With early detection, the right care, and a few lifestyle adjustments, you can slow progression, reduce complications, and stay in control of your health.
*National Kidney Foundation. (September 11, 2023) “Chronic Kidney Disease (CKD)” kidney.org
The information provided by Responsum Health is for educational purposes only and does not replace professional medical advice. Always talk with your healthcare provider before making changes to your treatment or care. Responsum Health does not endorse specific treatments, providers, or products.
Source: {{articlecontent.article.sourceName}}
Receive daily updated expert-reviewed article summaries. Everything you need to know from discoveries, treatments, and living tips!
Already a Responsum member?
Available for Apple iOS and Android
Add Comments
Cancel