Responsum for CKD
{{user.displayName ? user.displayName : user.userName}}
{{ user.userType }}

National Kidney Foundation
Learn how hemodialysis works, your treatment options, and what to expect—so you can feel more confident managing kidney failure.
Hearing that your kidneys have stopped working can feel overwhelming. If you’re in this situation, you’re not alone and you do have options.
Hemodialysis is one of the most common treatments for kidney failure. While it may sound intimidating at first, understanding how it works and what your choices are can help you feel more in control of your care. This article combines guidance from the National Kidney Foundation with practical insights to help you navigate what comes next.*
Hemodialysis is a treatment that takes over some of the work your kidneys can no longer do. Its main job is to remove waste, extra fluid, and toxins from your blood.
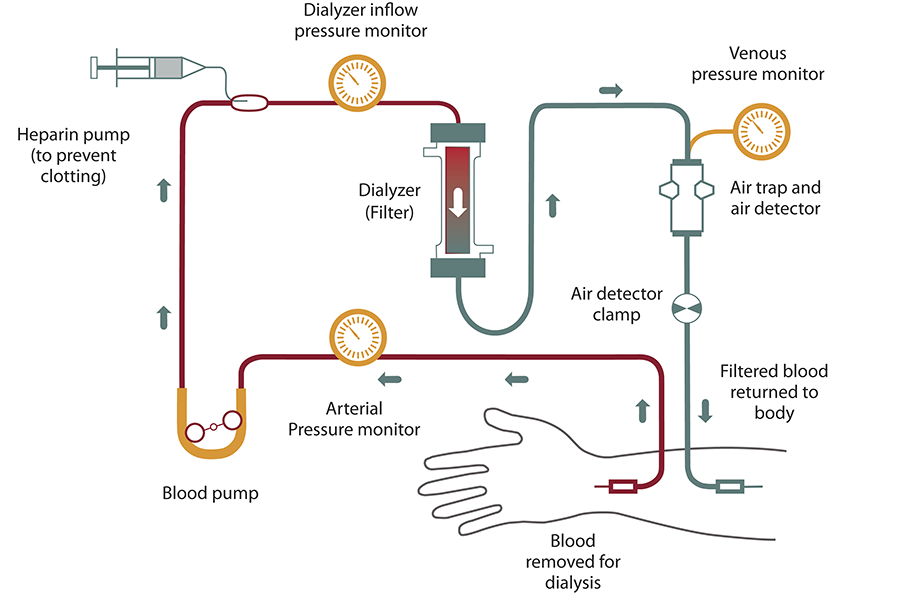
Here’s how it works:
Only a small amount of blood is outside your body at any time, and the machine carefully controls things like fluid removal, pressure, and treatment time .
This process may sound complex, but over time, many patients become very familiar and even comfortable with it.
You have two main options: in-center dialysis or home dialysis. Each has its own benefits, depending on your lifestyle, health needs, and comfort level.
This is the most common option. You go to a dialysis center where trained staff handle your treatment.
This option works well if you prefer having medical staff handle everything or if you’re not comfortable managing treatment yourself.
With home dialysis, you (and usually a care partner) are trained to perform treatments at home.
This option gives you more flexibility and control over your schedule. Research also shows that patients who are more involved in their care often feel better and do better overall.
However, it does require:
If you choose home dialysis, there are a few different ways to do it. Your doctor will help you decide what fits best with your health and daily life.
Because treatments are more frequent, less fluid is removed each time. This often means fewer side effects like cramping, nausea, or feeling “wiped out” afterward.
Longer, slower treatments allow for more gentle fluid removal and better waste clearance.
Some patients may even combine different approaches, depending on their needs.
Many patients who switch to home dialysis—or to more frequent treatments—report meaningful improvements in how they feel.
These may include:
Of course, results vary from person to person—but these benefits are a big reason more patients are exploring home options.
Dialysis machines have come a long way. Newer systems are:
This means your care team may be able to track your treatments from a distance, adding an extra layer of support.
If you’re considering home dialysis, it’s worth asking your doctor about the latest equipment available.
Home dialysis isn’t the best choice for everyone—and that’s okay.
You may be a good candidate if:
You may prefer in-center dialysis if:
There’s no “one-size-fits-all” answer here. The best choice is the one that fits your life, your health, and your comfort level.
The good news is that dialysis is typically covered by insurance, including Medicare.
Medicare may cover part of:
You may qualify if:
If you have employer insurance, it may be your primary coverage for the first 30 months, with Medicare as secondary.
A social worker at your dialysis center can help you understand your specific coverage and any additional costs.
Starting hemodialysis is a big life change, but it doesn’t mean you lose control. In fact, the more you learn and stay involved, the more empowered you can feel.
Whether you choose in-center care or explore home dialysis, there are options that can fit your life. With the right support, education, and care team, many people live full and meaningful lives on dialysis.
*National Kidney Foundation. (2020, Apr. 16). “Home Hemodialysis” kidney.org
The information provided by Responsum Health is for educational purposes only and does not replace professional medical advice. Always talk with your healthcare provider before making changes to your treatment or care. Responsum Health does not endorse specific treatments, providers, or products.
Source: {{articlecontent.article.sourceName}}
Receive daily updated expert-reviewed article summaries. Everything you need to know from discoveries, treatments, and living tips!
Already a Responsum member?
Available for Apple iOS and Android
Add Comments
Cancel